Capsule Endoscopy for Crohn's Disease: A Patient Guide

This article is for informational purposes only and does not constitute medical advice. Always consult your healthcare provider before making any changes to your treatment plan.
If your gastroenterologist has mentioned capsule endoscopy for Crohn's disease, you might be wondering what it actually involves - and whether swallowing a tiny camera is as strange as it sounds. For many of us living with Crohn's, the small bowel is the hardest part of the gut to monitor, sitting beyond the reach of a standard colonoscope. Capsule endoscopy was designed to solve exactly that problem, and understanding how it works can help you walk into the appointment feeling prepared rather than anxious.
Key Takeaways
- A 2024 network meta-analysis of 29 studies ranked video capsule endoscopy first among small bowel imaging modalities, with 89.6% sensitivity and 86.2% specificity for diagnosing Crohn's disease (2).
- The overall capsule retention rate in Crohn's disease is 3.32%, and pre-screening with a dissolvable patency capsule can reduce that risk further (1).
- The PillCam Crohn's Capsule features two wide-angle cameras and up to 14-hour battery life, imaging both the small bowel and colon in a single procedure (5).
- Combined capsule endoscopy plus ileocolonoscopy detected 97.3% of inflammatory lesions, compared with 57.3% for older barium-based imaging plus colonoscopy (4).
- Capsule endoscopy is especially valuable when colonoscopy and cross-sectional imaging give conflicting results or when proximal small bowel disease is suspected.
What Is Capsule Endoscopy and Why Is It Used in Crohn's Disease?
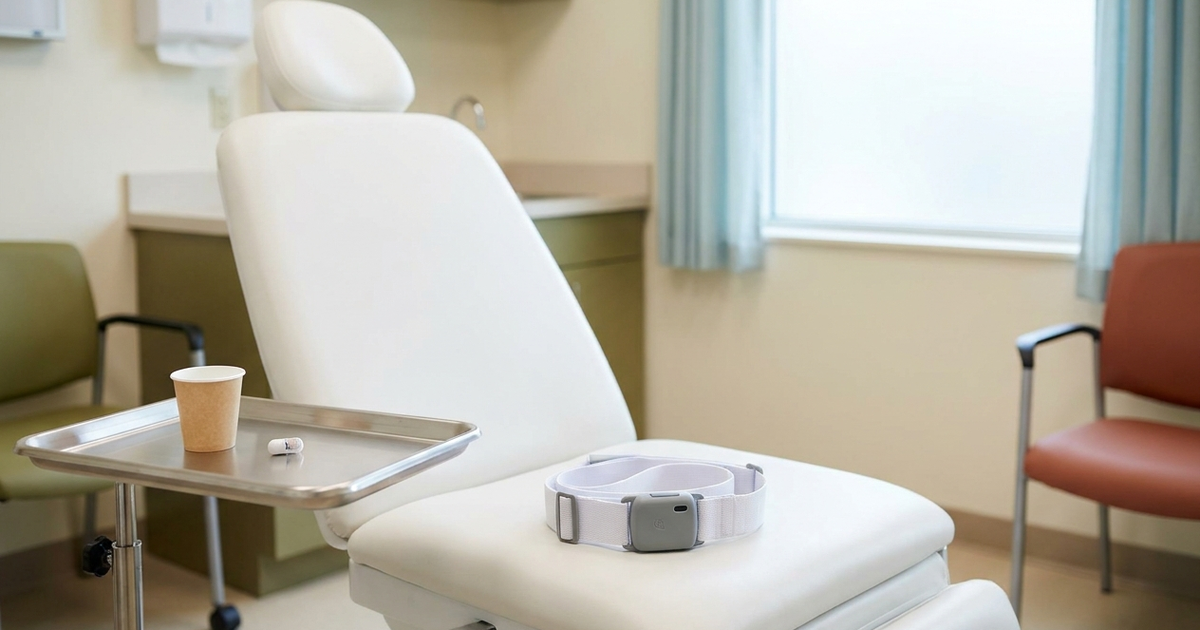
Capsule endoscopy uses a pill-sized swallowable camera - about the size of a large vitamin - that captures images of the digestive tract as it travels naturally through the body, typically passing within 24 hours (7). It was developed specifically to visualize the small intestine, the region most commonly affected by Crohn's disease and the most difficult to reach with conventional endoscopes.
How the Capsule Camera Works
Once you swallow the capsule with a sip of water, it begins taking roughly 2 images per second as peristalsis propels it through your digestive system. Over the course of the exam, it captures around 10,000 images in total (7). A small recording device worn on a belt around your waist collects the data wirelessly. After the recording period, you return the device and your gastroenterologist reviews the images using specialized software.
The procedure itself is painless. You go about your normal day while the capsule does its work - no sedation, no scope, no recovery time.
PillCam Crohn's Capsule (PCC) vs Standard Small Bowel Capsule
Standard small bowel capsule endoscopy (SBCE) focuses exclusively on the small intestine. It is excellent for finding subtle mucosal changes - tiny ulcers, aphthous lesions, early inflammation - that cross-sectional imaging can miss.
The PillCam Crohn's Capsule (PCC) is a newer, panenteric device designed specifically for Crohn's patients. It features two adjustable frame-rate wide-angle cameras and an extended battery life of up to 14 hours, allowing it to image both the small bowel and colon in a single procedure (5). Your gastroenterologist may use the Eliakim score - a validated scoring system developed for the PCC - to grade the severity of Crohn's findings across the entire gut (5). This panenteric approach can be particularly useful when a complete picture of disease extent is needed without requiring a separate colonoscopy.
How Capsule Endoscopy Compares to MRE, Ultrasound, and Other Tests
For patients already familiar with imaging tools like MR enterography or intestinal ultrasound, a natural question is where capsule endoscopy fits in. The short answer is that it excels at finding subtle small bowel disease that other modalities may miss.
Diagnostic Sensitivity and Specificity
A 2024 network meta-analysis pooling 29 studies and 2,609 patients ranked video capsule endoscopy first among all small bowel imaging modalities for diagnosing Crohn's disease. It achieved a sensitivity of 89.6% and specificity of 86.2% (2). In comparison, MR enterography reached 82% sensitivity and 71.6% specificity, CT enterography showed 79.6% sensitivity and 82.7% specificity, and intestinal ultrasound had 89.3% sensitivity with 72% specificity in the same analysis (2).
A separate review reinforced these findings, reporting that capsule endoscopy detected active enteric inflammation in 94% of cases compared with 22% for MRE in one head-to-head comparison, and 76.6% versus 44.7% in another (6). These are striking differences, especially for patients whose disease is concentrated in the proximal small bowel where other tools may have limited visibility.
Strengths in Proximal Small Bowel Disease
Capsule endoscopy is particularly strong at identifying subtle proximal small bowel lesions - inflammation in the jejunum or upper ileum - that cross-sectional imaging can overlook (4). If your colonoscopy shows a clean terminal ileum but you are still experiencing symptoms, or if your fecal calprotectin remains elevated without an obvious source, capsule endoscopy may reveal disease that has been hiding upstream.
When combined with ileocolonoscopy, capsule endoscopy detected 97.3% of inflammatory lesions, compared with 57.3% for traditional small bowel follow-through plus ileocolonoscopy (4). That is a dramatic improvement in diagnostic yield.
Capsule Retention: The Main Risk and How Doctors Prevent It
The most significant risk specific to capsule endoscopy is retention - the capsule becoming lodged in the bowel, usually at a stricture or narrowing. Understanding this risk and how your doctor can minimize it is key to feeling confident about the procedure.
What Capsule Retention Means
Capsule retention means the camera does not pass naturally and remains stuck in the intestine. A meta-analysis by Pasha and colleagues found that the overall capsule retention rate in Crohn's disease is 3.32% (95% CI 2.62-4.2%). The risk is higher in patients with established Crohn's (4.63%) than in those with suspected but unconfirmed disease (2.35%), and lower in children (1.64%) than in adults (3.49%) (1).
In most cases, a retained capsule can be retrieved endoscopically. In rare instances, surgical removal is needed. The capsule itself is not harmful while retained, but it does need to come out eventually, and you cannot have an MRI while it is still inside your body.
The Patency Capsule Pre-Screen
This is where the patency capsule comes in - and it is something many patients are not told about until the day of the procedure. The Agile Patency Capsule (FDA-approved in 2006) is a same-size dummy capsule made of dissolvable material. You swallow it before the real capsule, and if it passes through without getting stuck, your doctor knows the path is clear (6).
A 2025 systematic review of 23 studies involving 3,273 patients found that the patency capsule has a sensitivity of 75% and specificity of 94% for predicting retention, with a false-negative rate of only 2.7% (3). This is significantly more reliable than relying on cross-sectional imaging alone to assess stricture risk.
With a patency capsule pre-screen, retention rates in established Crohn's disease drop from 4.63% to 2.88% (1), and in some centers the rate falls even further - as low as 0.39% in a Japanese multicenter cohort (4). If your gastroenterologist does not mention patency testing, it is worth asking about it directly.

What to Expect: Preparation, the Procedure, and Reading Results
Knowing what the day looks like from start to finish can take a lot of the uncertainty out of the experience.
Bowel Prep and the Day Of
Preparation for capsule endoscopy is similar to colonoscopy prep, though specific instructions vary by center. In general, you will follow a clear liquid diet the day before the procedure, take a bowel preparation solution to clean out the intestines, and fast overnight. A clean bowel means clearer images, so following the prep instructions closely makes a real difference in the quality of the results.
On the morning of the procedure, you will arrive at the clinic, have the recording belt fitted, and swallow the capsule with water. The whole setup takes about 15 minutes, and then you are free to leave.
Wearing the Recorder and Getting Your Results
You wear the small recording device on a belt or harness for 8 to 14 hours, depending on whether you are using a standard small bowel capsule or the panenteric PillCam Crohn's Capsule. During this time, you can go about most of your normal activities - no sedation means no recovery period. You will be asked to avoid eating for a few hours after swallowing the capsule and then gradually resume a light diet.
After the recording period, you return the device to the clinic. Your gastroenterologist reviews the images using reading software (the PCC uses Rapid 9 software) and may assign a severity score based on what is found (5). Results typically take a few days to a week, depending on your center.
A few important safety notes: do not have an MRI until you have confirmed the capsule has passed (watch your stool or have an abdominal X-ray if there is any doubt), and contact your doctor promptly if you develop severe abdominal pain after swallowing the capsule.
When Capsule Endoscopy Is the Right Choice for Crohn's Patients
Capsule endoscopy is not the right tool for every situation, but when it fits, it provides information that no other test can match. Understanding when it is most useful - and when another approach might be better - helps you have a more productive conversation with your care team.
Common Indications
Your gastroenterologist may recommend capsule endoscopy to diagnose suspected Crohn's disease when colonoscopy is normal but symptoms persist, evaluate the full extent of disease in known Crohn's, assess mucosal healing during treatment, or investigate obscure gastrointestinal bleeding (7). It is also endorsed by international guidelines from the ESGE, Asia Pacific, and Japanese societies as part of the diagnostic pathway for both established and suspected Crohn's disease (4).
Capsule endoscopy is especially helpful during treatment monitoring. If you and your doctor want to confirm that a biologic or immunosuppressant is actually healing the mucosa - not just improving symptoms - capsule endoscopy provides direct visual evidence of the small bowel lining. As we explored in our guide on understanding flares and remission, achieving mucosal healing is increasingly recognized as the gold standard treatment target.
When Another Test Might Be Better
Capsule endoscopy is not ideal when strictures or fistulas are already suspected, since the retention risk may outweigh the benefit. In those situations, MR enterography or CT enterography can map stricture anatomy, fistula tracts, and extra-intestinal complications like abscesses without any retention risk. Intestinal ultrasound is another excellent option for quick, point-of-care assessments, particularly for terminal ileum disease.
In practice, these tools often complement each other rather than compete. Your care team may use capsule endoscopy for detailed mucosal assessment and MRE for transmural and extra-luminal imaging, combining results for a complete picture.
Questions to Ask Your Gastroenterologist
Walking into an appointment with specific questions helps you make the most of your time and feel more in control of the process. Here are questions worth raising:
- Do I need a patency capsule first, and what is my retention risk based on my imaging history and disease location?
- Will I be having a standard small bowel capsule or the PillCam Crohn's Capsule?
- What scoring system will you use to grade my findings - for example, the Eliakim score for panenteric assessment (5)?
- How will the capsule endoscopy results change or inform my treatment plan?
- Should we combine capsule endoscopy with MRE or intestinal ultrasound for a more complete picture?
- What should I do if the capsule does not pass naturally, and how will we confirm it has?
Your care team wants you to understand your diagnostic pathway. Asking these questions signals that you are an informed, engaged partner in your own care.
Frequently Asked Questions
Is capsule endoscopy painful?
No. The capsule is about the size of a large vitamin and is swallowed with water just like a pill. There is no sedation, no insertion of instruments, and no recovery time. Most patients describe the experience as surprisingly easy. The recording belt can feel slightly bulky, but it is not uncomfortable for most people.
How long does the capsule endoscopy procedure take?
The setup at the clinic takes about 15 minutes. You then wear the recording device for 8 to 14 hours depending on the capsule type - standard small bowel capsules record for about 8 hours, while the PillCam Crohn's Capsule can record for up to 14 hours (5). You can go about your normal activities during this time.
What happens if the capsule gets stuck?
Capsule retention occurs in approximately 3.32% of Crohn's patients overall (1). If it happens, the capsule is most often retrieved endoscopically. In rare cases, surgical removal may be needed. A patency capsule pre-test can significantly reduce this risk. Contact your doctor if you experience severe abdominal pain after the procedure.
Can capsule endoscopy replace colonoscopy for Crohn's monitoring?
Not entirely. Colonoscopy remains essential for biopsy collection and direct visualization of the colon and terminal ileum. However, capsule endoscopy provides superior imaging of the proximal small bowel that colonoscopy cannot reach. Many gastroenterologists use both tools together for comprehensive monitoring - combined capsule endoscopy and ileocolonoscopy detected 97.3% of inflammatory lesions (4).
Is a patency capsule always required before capsule endoscopy?
Not always, but it is strongly recommended for patients with known or suspected strictures. Guidelines vary by center and by your individual risk profile. A 2025 review found that patency capsule screening has 94% specificity for predicting safe passage (3). If your doctor does not mention it, ask whether a patency test is appropriate for your situation.
Does insurance cover capsule endoscopy?
Coverage varies widely depending on your country, insurance plan, and clinical indication. In many healthcare systems, capsule endoscopy is covered when there is a documented clinical need - such as suspected small bowel Crohn's disease that other tests have not confirmed. Contact your insurance provider or healthcare system before the procedure to understand costs and pre-authorization requirements.
Should I ask for capsule endoscopy if my colonoscopy looks normal but I still have symptoms?
This is one of the most common and appropriate indications for capsule endoscopy. Crohn's disease can affect the proximal small bowel beyond the reach of a colonoscope, and a normal colonoscopy does not rule out small bowel involvement. If your symptoms persist and inflammatory markers like fecal calprotectin remain elevated, discuss capsule endoscopy with your gastroenterologist as a next step.
References
- Pasha, S.F., et al. Capsule Retention in Crohn's Disease: A Meta-analysis. Inflammatory Bowel Diseases, 2020. View on PubMed
- A network meta-analysis of capsule endoscopy versus imaging modalities for diagnosing small bowel Crohn's disease. 2024. View on PubMed
- Patency Capsule and Cross-Sectional Imaging for Predicting Capsule Endoscopy Retention: A Systematic Review and Meta-Analysis. 2025. View on PubMed
- Capsule Endoscopy in Inflammatory Bowel Disease: Current Status and Future Directions. 2025. Read article
- A novel PillCam Crohn's capsule score (Eliakim score) for the assessment of severity of Crohn's disease. 2020. Read article
- The Role of Capsule Endoscopy in Crohn's Disease: A Review. 2022. Read article
- Cleveland Clinic. Capsule Endoscopy: Prep, Procedure, What It Can Diagnose. 2024. Read article
Recommended Resources
Browse ResourcesRelated Articles

Kidney Stones in Crohn's Disease: Causes and Prevention
Kidney stones affect Crohn's disease patients more often than the general population. Learn the main causes, risk factors, and proven prevention strategies.

Bile Acid Diarrhea in Crohn's: Causes and Treatment
Bile acid diarrhea affects more than 30% of Crohn's disease patients yet often goes undiagnosed. Learn the symptoms, SeHCAT testing, and treatment options.
Endoscopic Balloon Dilation for Crohn's Strictures Guide
Endoscopic balloon dilation for Crohn's strictures offers a minimally invasive alternative to surgery. Learn success rates, risks, and patient outcomes.

Vaccines for Crohn's Disease: What Patients Need to Know
Vaccines for Crohn's disease patients matter most before you start biologics. Learn which shots are safe, which ones to avoid, and how to time them right.

Preventing Postoperative Crohn's Recurrence: 2026 Guide
Up to half of Crohn's patients face endoscopic recurrence within a year of surgery. Learn 2026 evidence-based ways to prevent postoperative recurrence.
MR Enterography for Crohn's Disease: A Patient's Guide
MR enterography for Crohn's disease is a radiation-free scan that maps small bowel inflammation. Learn how MRE works, what to expect, and why it matters.