MR Enterography for Crohn's Disease: A Patient's Guide
This article is for informational purposes only and does not constitute medical advice. Always consult your healthcare provider before making any changes to your treatment plan.
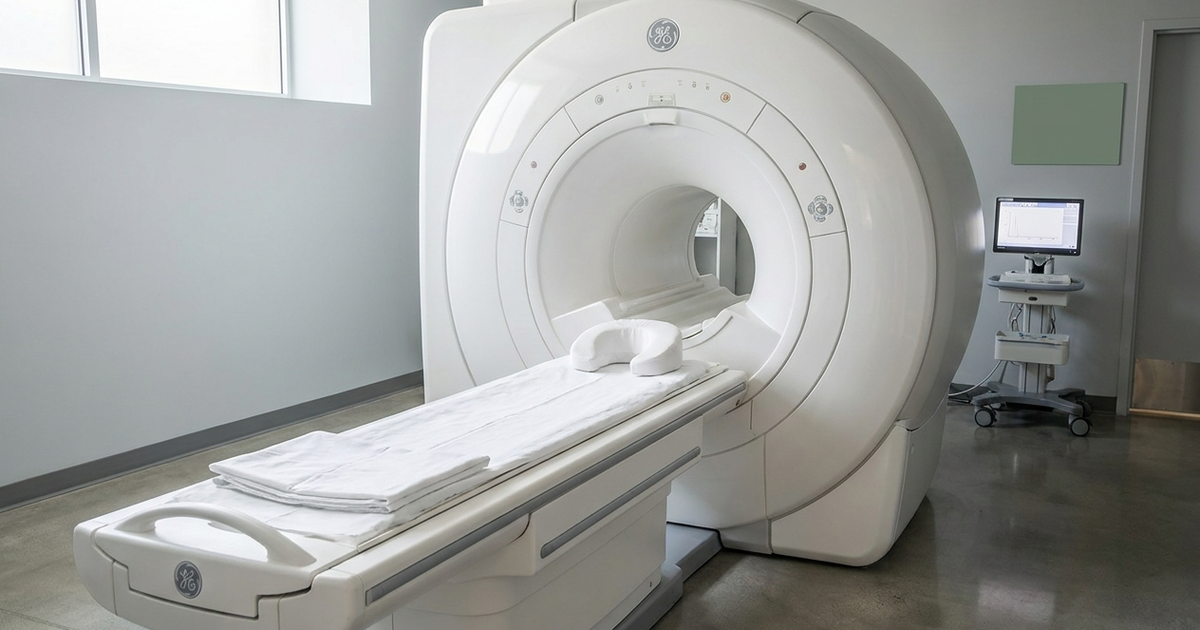
If you have been told you need an MR enterography for Crohn's disease, your first reaction might be a mix of curiosity and dread. What exactly is this scan? Will it hurt? What will it show? For many of us managing Crohn's, imaging appointments can feel like another stressful hurdle in a long list of medical obligations. The good news is that MRE is one of the most detailed and patient-friendly imaging tools available today - and understanding what to expect can take a lot of the anxiety out of the experience.
Key Takeaways
- MR enterography achieves 97 percent sensitivity and 96 percent specificity for detecting small bowel Crohn's disease, according to the landmark METRIC trial (1).
- Unlike CT enterography, MRE uses no ionizing radiation, making it safer for the repeated scans Crohn's patients often need over a lifetime (3)(4).
- MRE can distinguish active inflammation from fibrosis with approximately 90 to 98 percent accuracy, which directly influences whether treatment is medical therapy or surgery (2).
- The scan itself takes 30 to 45 minutes, but plan for extra time to drink roughly 1,000 to 1,350 mL of oral contrast beforehand (4).
- Society of Abdominal Radiology consensus recommends cross-sectional enterography at initial Crohn's diagnosis and for ongoing small bowel monitoring (3).

What MR Enterography Is and Why It Matters for Crohn's Disease
MR enterography is a specialized type of MRI designed to produce detailed images of the small bowel. It combines a dedicated imaging protocol with oral contrast (to distend the intestines) and intravenous gadolinium contrast (to highlight inflamed tissue), giving radiologists a clear picture of the intestinal wall and surrounding structures (4). Think of it as an MRI that has been fine-tuned specifically for the gut.
MRE vs. Regular MRI and CT Enterography
A standard abdominal MRI gives a general view of your organs but is not optimized for the bowel. MRE uses a specific oral contrast agent - typically dilute barium with sorbitol or a polyethylene glycol (PEG) solution - to fill and stretch the small intestine so the walls can be seen clearly. Without this distension, small bowel disease can easily be missed.
CT enterography (CTE) provides similar diagnostic information to MRE, and in some centers it remains the more available option. The key difference is radiation. CT scans use ionizing radiation, and for a disease that often requires repeated imaging over decades, that cumulative exposure matters (3)(4). MRE delivers the same level of detail without any radiation dose, which is why it has become the preferred cross-sectional imaging tool for long-term Crohn's monitoring.
Where does MRE fit alongside other tools? It complements intestinal ultrasound, which is excellent for quick, point-of-care assessments, and endoscopy, which remains essential for biopsy and direct mucosal visualization. Together, these form a modern monitoring toolkit that your care team can draw from depending on the clinical question.
Why No Ionizing Radiation Is a Big Deal for Lifelong Monitoring
Crohn's disease is typically diagnosed in young adults, and many patients will need imaging studies repeatedly over the course of their lives. A 2025 review emphasized that MRE's radiation-free nature makes it particularly well suited for this scenario, allowing clinicians to monitor disease activity and treatment response without adding to a patient's lifetime radiation burden (2). For younger patients and anyone requiring frequent scans, this is a meaningful safety advantage.
What MRE Can Show in Crohn's Disease
One of the most valuable aspects of magnetic resonance enterography is the depth of information it provides. It does not just show whether inflammation is present - it helps characterize what kind of disease is happening.
Active Inflammation, Strictures, and Fibrosis
MRE can detect thickening of the bowel wall, swelling (edema), increased blood flow to the intestinal lining (mucosal enhancement), and ulceration. These findings together paint a picture of active inflammatory disease.
Critically, MRE can help distinguish between strictures caused by active inflammation and those caused by fibrosis (scarring). A 2025 review reported that MRE achieves approximately 90 to 98 percent diagnostic accuracy in making this distinction (2). This matters enormously for treatment decisions: inflammatory strictures may respond to medications like biologics, while fibrotic strictures are more likely to require surgical intervention.
Penetrating Disease - Fistulas, Abscesses, and Beyond
Crohn's can cause complications that extend beyond the bowel wall itself. Fistulas (abnormal tunnels connecting the bowel to other organs or the skin), abscesses (pockets of infection), and sinus tracts are all penetrating complications that MRE excels at detecting (2). Identifying these changes early can fundamentally alter treatment plans, sometimes making the difference between managing a complication medically and needing urgent surgery.
MRE also reveals extra-intestinal findings such as enlarged lymph nodes, changes in the mesenteric fat surrounding the bowel, and detailed imaging of perianal disease - all of which contribute to a more complete understanding of your disease.
How Accurate Is MRE? What the Research Shows
For patients weighing their options, the data on MRE accuracy is reassuring.
Sensitivity, Specificity, and the METRIC Trial
The METRIC trial is one of the most important studies comparing imaging approaches for Crohn's disease. It found that MR enterography achieved 97 percent sensitivity and 96 percent specificity for detecting small bowel Crohn's disease (1). A 2025 review confirmed these strong numbers, reporting overall MRE accuracy near 90 percent, with sensitivity around 97 percent and specificity over 95 percent for IBD detection across multiple studies (2).
In practical terms, this means MRE is very good at finding disease when it is there (high sensitivity) and very good at confirming you are clear when you are actually in remission (high specificity).
MRE vs. Intestinal Ultrasound
The METRIC trial also compared MRE with intestinal ultrasound (IUS), which showed 92 percent sensitivity and 84 percent specificity in the same patient group (1). Both are excellent tools, and both are supported by ECCO and STRIDE-II guidelines as first-line monitoring options (1). The practical difference is that MRE tends to be stronger for staging the full extent and complexity of disease - especially in the deeper small bowel - while intestinal ultrasound shines as a quick, accessible, point-of-care tool.
Your gastroenterologist may use both at different times depending on the clinical question. If you have previously had a fecal calprotectin test that suggests active inflammation, MRE can provide the detailed mapping to figure out exactly where and how severe that inflammation is.
Understanding MRE Activity Scores
Radiologists use validated scoring systems to quantify what they see on MRE. The most widely used include the MaRIA score, simplified MaRIA (sMaRIA), Clermont score, and London score (6). These systems standardize reporting by assigning numerical values based on wall thickness, contrast enhancement, edema, and ulceration. If your report mentions one of these scores, it is a sign that your radiologist is using an evidence-based framework to grade your disease activity - which helps your gastroenterologist make more precise treatment decisions.
Preparing for an MRE Scan: What to Expect
Knowing the practical details can help you feel more in control on scan day.
Before the Scan
You will typically need to fast for 4 to 6 hours before the exam (4). On arrival, you will be asked to drink approximately 1,000 to 1,350 mL of oral contrast over roughly 45 minutes (4). The contrast is usually a dilute barium-sorbitol or PEG-based solution, and its job is to fill and distend your small intestine so the walls show up clearly on imaging. The taste varies by center - some patients describe it as mildly unpleasant, others say it is tolerable with small, steady sips.
During the Scan
You will lie on a table that slides into the MRI scanner. The scan itself takes around 30 to 45 minutes. At some point during the procedure, an IV line will deliver gadolinium contrast to help highlight areas of inflammation. You may also receive a small injection of glucagon, which temporarily slows bowel movement and reduces motion artifacts in the images (4).
For those who experience claustrophobia, it is worth knowing that open MRI scanners are available at some centers, and mild sedation can be arranged. Many facilities allow you to listen to music during the scan, which can make the time pass more comfortably. The scanner is loud - earplugs or headphones are standard.
After the Scan
The most common aftereffect is frequent bowel movements for a few hours, caused by the large volume of oral contrast working its way through your system. Some patients also report mild bloating or a heavy feeling in the stomach. These effects are temporary and typically resolve within the same day. Results are usually reviewed by a radiologist and sent to your gastroenterologist within a few days.
When Doctors Order MRE for Crohn's
Understanding why your doctor has ordered an MRE can help you feel more engaged in your own care. Common scenarios include:
- At initial diagnosis - to map small bowel involvement in areas that endoscopy cannot reach (3). Since colonoscopy only visualizes the colon and terminal ileum, MRE fills the gap for the rest of the small intestine.
- Monitoring treatment response - to assess whether biologics, immunomodulators, or other therapies are reducing inflammation (2)(5). This is especially relevant for treatment intensification decisions.
- Suspected complications - new or worsening pain, signs of obstruction, or concerns about fistulas and abscesses warrant detailed imaging (2).
- Before surgery - to map disease extent and precisely locate strictures or fistulas so the surgical team can plan accordingly (3).
- When other tests are inconclusive - if fecal calprotectin or symptoms suggest active disease but endoscopy appears normal, MRE can reveal small bowel inflammation that is otherwise hidden.
Limitations, Risks, and Practical Considerations
Like any medical tool, MRE has trade-offs worth understanding.
Cost and insurance - MRE is typically more expensive than CT enterography or intestinal ultrasound, and many insurance plans require prior authorization. In different healthcare systems worldwide, access and out-of-pocket costs vary considerably - ask your care team about what to expect in your region.
Claustrophobia and motion - lying still in a narrow scanner for 30 to 45 minutes is challenging for some patients. Motion artifacts can reduce image quality, so ask about open MRI or sedation options if this is a concern.
Gadolinium contrast - the IV contrast used in MRE carries a rare risk of allergic reaction. There is also ongoing research into long-term gadolinium retention in the body, though no harmful effects have been established in patients with normal kidney function. Your radiology team will screen for kidney issues before administering it.
Pregnancy - MRE is generally avoided during pregnancy, particularly in the first trimester. If you are pregnant or planning to become pregnant and need imaging, discuss alternatives such as intestinal ultrasound with your care team.
Oral contrast matters - the quality of your images depends heavily on completing the oral contrast. Drinking the full volume can feel uncomfortable, especially if you are dealing with active flare symptoms, but it is essential for an accurate diagnosis.
Reading your report - if you review your MRE results, you may encounter terms like MaRIA score, wall thickness in millimeters, mural hyperenhancement, or mesenteric stranding. These are standardized descriptors that help quantify your disease activity. Do not hesitate to ask your gastroenterologist to walk you through the report - understanding your own imaging empowers better conversations about your care.
Frequently Asked Questions
Is MR enterography painful?
MRE itself is not painful. The most uncomfortable parts for most patients are drinking the oral contrast solution beforehand and lying still in the scanner for 30 to 45 minutes. Some people experience mild bloating from the oral prep. The IV contrast injection feels like a brief pinch, similar to a standard blood draw.
How is MRE different from a regular MRI?
MR enterography uses a specialized protocol with oral contrast to distend the small intestine and IV gadolinium to highlight inflammation. A standard abdominal MRI does not include these steps and is not optimized to evaluate bowel wall detail. MRE is specifically designed for Crohn's disease imaging and small bowel assessment.
Does MRE use radiation?
No. MRE uses magnetic fields and radio waves, not ionizing radiation. This is one of its biggest advantages over CT enterography for Crohn's patients who need repeated imaging over their lifetime (3)(4).
How long does the entire MRE appointment take?
Plan for approximately 2 to 3 hours total. This includes about 45 minutes to drink the oral contrast, 30 to 45 minutes for the scan itself, and time for check-in, IV placement, and any waiting between steps. The imaging portion is usually the shorter part of the visit.
Can MRE replace colonoscopy?
MRE and colonoscopy serve different roles. MRE excels at visualizing the small bowel and detecting complications like strictures, fistulas, and abscesses. Colonoscopy remains necessary for direct mucosal visualization, biopsy, and colorectal cancer surveillance. Many patients benefit from both at different points in their care.
Is MRE covered by insurance?
In many countries and insurance plans, MRE is covered when ordered for a confirmed or suspected diagnosis of Crohn's disease, though prior authorization is often required. Coverage varies significantly by region and plan - check with your insurance provider and ask your care team to submit the request with appropriate clinical documentation.
What should I ask my doctor about MRE?
Useful questions include: Why is MRE the best imaging option for me right now? Will I receive gadolinium contrast, and are there any risks given my kidney function? How will the results influence my treatment plan? Is an open MRI or sedation available if I am claustrophobic? Your doctor should be happy to walk you through these details.
References
- Kumar S, De Kock I, Blad W, Hare R, Pollok R, Taylor SA. Magnetic Resonance Enterography and Intestinal Ultrasound for the Assessment and Monitoring of Crohn's Disease. Journal of Crohn's and Colitis, 2024. Read study
- Mirica RE, Matura TF, Craciun E, Pavel D. The Importance of Magnetic Resonance Enterography in Monitoring Inflammatory Bowel Disease: A Review of Clinical Significance and Current Challenges. 2025. View on PubMed
- Bruining DH, Zimmermann EM, Loftus EV Jr, Sandborn WJ, Sauer CG, Strong SA. Consensus Recommendations for Evaluation, Interpretation, and Utilization of Computed Tomography and Magnetic Resonance Enterography in Patients With Small Bowel Crohn's Disease. Radiology, 2018. Read study
- RadiologyInfo.org. MR Enterography - Patient Information. 2024. Read article
- Lichtenstein GR, Loftus EV, Afzali A, Long MD, Barnes EL, Isaacs KL, Ha CY. ACG Clinical Guideline: Management of Crohn's Disease in Adults. 2025. View on PubMed
- Comprehensive Review of Magnetic Resonance Enterography-Based Activity Scoring Systems for Crohn's Disease. Investigative Magnetic Resonance Imaging, 2024. Read study
Recommended Resources
Browse ResourcesRelated Articles

Kidney Stones in Crohn's Disease: Causes and Prevention
Kidney stones affect Crohn's disease patients more often than the general population. Learn the main causes, risk factors, and proven prevention strategies.

Bile Acid Diarrhea in Crohn's: Causes and Treatment
Bile acid diarrhea affects more than 30% of Crohn's disease patients yet often goes undiagnosed. Learn the symptoms, SeHCAT testing, and treatment options.
Endoscopic Balloon Dilation for Crohn's Strictures Guide
Endoscopic balloon dilation for Crohn's strictures offers a minimally invasive alternative to surgery. Learn success rates, risks, and patient outcomes.

Vaccines for Crohn's Disease: What Patients Need to Know
Vaccines for Crohn's disease patients matter most before you start biologics. Learn which shots are safe, which ones to avoid, and how to time them right.

Preventing Postoperative Crohn's Recurrence: 2026 Guide
Up to half of Crohn's patients face endoscopic recurrence within a year of surgery. Learn 2026 evidence-based ways to prevent postoperative recurrence.

Capsule Endoscopy for Crohn's Disease: A Patient Guide
Capsule endoscopy for Crohn's disease uses a tiny swallowable camera to image the entire small bowel. Learn how PillCam works, what to expect, and the risks.